- Probartak Sangha Building (4th and 5th Floor), Probartak Circle, Panchlaish, Chittagong
- Phone: 01839392525, 01768225275,
- Emails: info.chittagong@bdeyehospital.com
- Hotline:01839392525
The department of Uveitis and ocular immunology is enriched with our qualified uveitis specialists. It deals with the whole battery of ocular inflammations including autoimmune diseases and infections in both adults and children.
The Uveitis & Ocular Immunology Service provides a multidisciplinary approach to the treatment of ocular inflammatory disease and other infectious disorders. Experts here deal with diagnosis and management of complex infectious and autoimmune diseases of the eye as well as eye diseases associated with various other systemic medical disorders. Our consultants are conversant with appropriate intervention techniques (like periocular or intraocular injections, lasers and surgeries if needed). In addition, we have the experience with the latest treatments including the use of immunosuppressive and immunomodulator for autoimmune eye diseases.
We co-ordinate with the other sub-specialties of ophthalmology and internal medicine efficiently to get the optimal treatment outcomes for patients with complex uveitic disorders.
WHAT IS UVEITIS?
Uvea is the middle part of the three coats of the eye. This further consists of the iris, ciliary body and the choroid. Inflammation of any of these parts is termed uveitis.
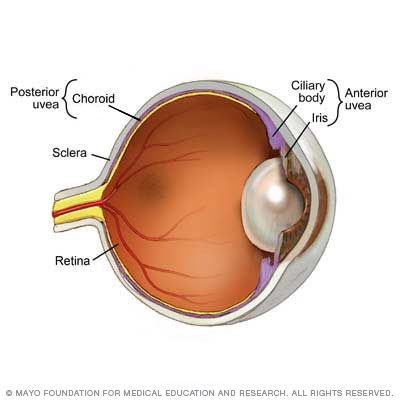
What are the types of uveitis?
Based on the part of the uvea involved, uveitis may be Anterior (involving the iris), Intermediate (involving the ciliary body), Posterior (involving the choroid) or Panuveitis (involving all the parts). There are different terms that people refer to uveitis, as iritis, scleritis, vitritis, choroiditis and chorioretinitis, however, each of them has different meanings.
What are the symptoms of uveitis?
Symptoms of uveitis are highly variable and may include any of the following: redness, pain, watering, inability to see bright light (photophobia), floaters (shadows moving across the field of vision), decreased vision and even loss of vision.
Uveitis can develop in any age. But it is more common in young to middle aged people.
What causes uveitis?
Uveitis occurs as a result of an immune reaction by our body to antigens (substances our body considers foreign). This reaction may occur against infectious agents (such as bacteria, fungi, viruses and even parasites), a wide range of autoimmune or inflammatory disorders (eg: spndyloarthropathy, juvenile idiopathic arthritis, sarcoidosis, systemic lupus erythematosus etc) that affects others parts of the body, some genetic transmissions, ocular injury, some drugs and very rarely some tumors or malignancy.
Among all of these, tuberculosis is one of the major causes for developing uveitis in any form.
In a small subset of patients, uveitis can occur due to undeterminable causes.
What investigations are uveitic patients required to undergo?
Uveitic patients often require a whole battery of investigations in order that the underlying cause of uveitis be determined and hence appropriately treated. These usually include blood and urine tests and/ or X rays. At times, a sample of the fluid from the patients’ eye may have to be subjected to lab tests.
As already discussed, uveitis can happen due to a wide range of diseases. So, based on patient’s symptoms and signs, investigations can be tailored as instructed by your doctor.
How is uveitis treated?
Steroids are the mainstay of treatment of uveitis. Depending on the location and the severity of the inflammation, they are used in the form of eye drops, eye ointment, injections around/ in the eye or injectable / oral route. Anterior uveitis is usually treated with topical steroids along with dilating eye drops, which help in reducing the pain associated with inflammation. These drops are to be used until the inflammation has completely subsided. The dose, strength and duration of the drops are determined by your doctor who decides the treatment in accordance to the amount of inflammation.
Injection of the steroid around the eye (periocular steroids) is used in certain cases of intermediate uveitis (or in macular edema as a consequence of uveitis). This results in slow release of the drug over a period of three to four weeks.
Oral steroids are often indicated in posterior/panuveitis.
Besides steroids, the other group of drugs used in the treatment of uveitis is immunosuppressives. These are especially reserved for patients intolerant to steroids, inflammation not resolving with only steroids and patients with certain systemic conditions like Behcet’s disease, Juvenile idiopathic arthritis, some cases of spondyloarthropathy, rheumatoid arthritis etc. The commonly used immunosuppressives include Methotrexate, Azathioprine, Cyclosporine, Mycophenolate mofetil, Cyclophosphamide and Biological agents. Now a days, biological agents are used to treat uveitis with associated various immunological diseases and noninfectious uveitis which are non-responsive to other medications. Infectious uveitis are treated with antibacterial, antifungal, antiprotozoal and antiviral agents.
What are the side effects of the drugs used in the treatment of uveitis?
Both steroids and immunosuppressives have side effects that are often not serious and reversible following the discontinuation of the drugs. But sometimes they may cause serious side effects. So, these drugs should always be taken as per your doctors’ instructions. Never start or stop these drugs of you own.
Topical steroids may cause cataract or an increase in the intraocular pressure (glaucoma). Oral steroids may cause acidity, increase in weight and rarely diabetes, hypertension, osteoporosis and nervousness/ depression.
Immunosuppressives may cause bone marrow depression that is reflected as a decrease in your blood counts. Some of them also interfere with the normal functions of the liver, cause mouth ulcers, rarely sterility and secondary malignancies. Thus, periodic blood counts/liver function tests may be required and will be advised by your doctor when on these drugs.
Women in the reproductive age group are advised not to become pregnant when on treatment with immunosuppressives/ oral steroids. If you develop any infection while on treatment you need to take appropriate antibiotics immediately after consulting your doctor. In case you require to undergo any surgical procedure while on these drugs, please inform your treating doctor about the same.
Will uveitis recur after treatment?
It is important to remember that uveitis is a recurrent condition and hence requires a prolonged and regular follow up with your doctor. Consult your ophthalmologist at the earliest signs of a recurrence. This will make treatment easier and resolution speedier.
What are the complications of uveitis?
Uveitic patients may develop corneal opacity (Band keratopathy), cataract (opacification of the lens), glaucoma (raised intraocular pressure), hypotony, vitreous haemorrhage, macular edema (swelling of the central part of the retina), retinal detachment or neovascularization in addition to the inflammation itself. These complications may require additional medical or surgical management.
Periodic follow up with Ophthalmologist and Internist may help you to early detection and treatment of ocular (eyes) complications as well as side effects of medicines.
Back To Top
© 2025 Bangladesh Eye Hospital. All Rights Reserved.
Design by AbacusIT.
Probartak Sangha Building (4th and 5th Floor), Probartak Circle, Panchlaish, Chittagong
01839392525, 01768225275

Cataract

None

None

None

None

None

None

None

None

None

Cataract

Cataract

Cataract

Cataract

Cataract

None

None

None

None

None

Cataract

Cataract

None

None

None

None

None

Cataract

Cataract

Cataract

Cataract

Cataract

Cataract

Cataract

None

Cataract

Cataract

Cataract

Cataract

Cataract

Cataract

None

None

Cataract

Cataract

None
Cataract

Cataract

Cataract

Cataract

None

Cataract

Cataract

Cataract

None

Cataract

Cataract
None

Cataract

Cataract

Cataract

Cataract

Cataract

Cataract

Cataract

None

None

None

None

Cataract

None

Cataract

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

Cataract

None

None

Cataract

None

None

Cataract

None

None

None

None

None

None

None

None

Cataract

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

Cataract

None

None

Cataract

Cataract

None

None

Cataract

Cataract

Cataract

Cataract

Cataract

None

Cataract

Cataract

Cataract

None

None

Cataract

Cataract
Cataract

None

Cataract

None

None

Cataract

None

None

None

None

None

None

None

Cataract

Cataract

Cataract

Cataract

Cataract

Cataract

None

None

None

None

None

None

None

None

None

Cataract

Cataract

Cataract

Cataract
None

Cataract

None

Cataract

Cataract

Cataract

Cataract

None

None

None

None

None

None

None

Cataract

None

None

None

None

None

None

None

None

None

None

None

Cataract

None

None

Cataract

Cataract

None

Cataract

None

None

None

None

None

None

Cataract

None

None

None

Cataract

Cataract

Cataract

Cataract

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

Cataract

Cataract

None

None

None

None

None

Cataract

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

None

One of our customer care executive will confirm your appointment by contacting with you within next 1-2 hours

Doctor Name: Dr. Collis Molate,
Appointment Date & Time:
Chamber Location: Bangladesh Eye Hospital, Branch
